A workplace head injury can change everything in an instant. At Robin J Peterson Company, LLC, we’ve helped countless workers navigate head injury workers compensation claims and secure the benefits they deserve.
This guide walks you through your rights, the claims process, and how to overcome common obstacles that stand between you and fair compensation.
What Head Injuries Look Like in the Workplace
Falls, impacts, and struck-by incidents dominate workplace head injuries. According to the National Council on Compensation Insurance, slips and falls, being struck by an object or person, and motor vehicle accidents drive more than 85 percent of traumatic brain injury medical costs in workers compensation claims. The construction industry accounts for the largest share of these injuries, representing 32 percent of all TBIs compared to 18 percent for all lost-time claims.
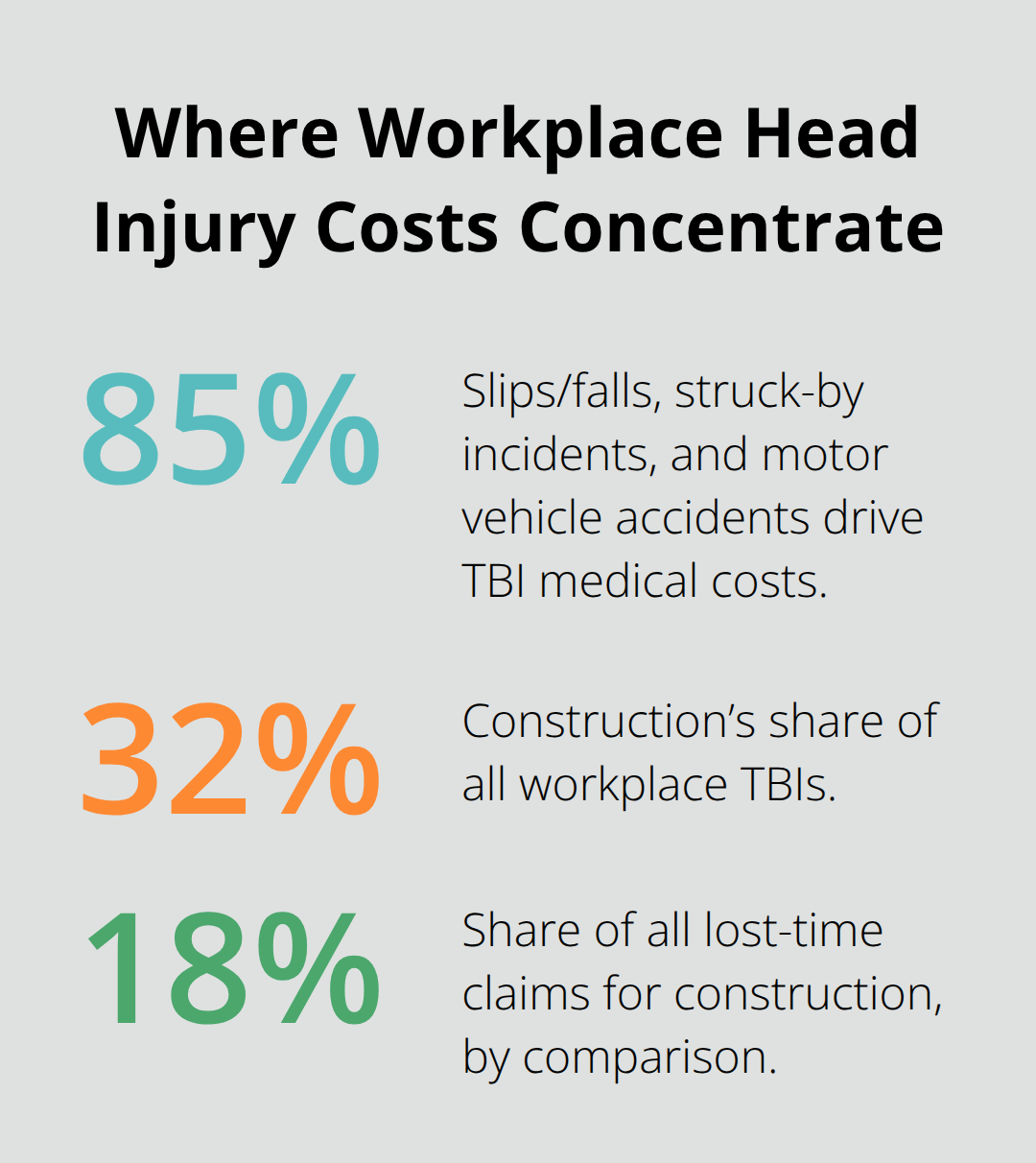
This concentration matters because it shows where prevention efforts should focus and why certain industries face higher claim costs.
Traumatic Brain Injuries from Impact Carry Severe Consequences
Traumatic brain injuries from falls and impacts represent the most severe end of the spectrum. When a worker falls from height or strikes their head on equipment, the resulting brain injury often requires immediate hospitalization and long-term care. The Bureau of Labor Statistics reported that roughly 83,000 workers experienced head injuries on the job in 2020, with about 13 percent needing at least one month away from work. What makes TBIs particularly expensive is their medical trajectory. Hospital inpatient stays for TBIs average longer than other injuries, with about 10 percent lasting 30 days or more. Roughly 8 percent of inpatient TBI stays include surgery, which significantly increases total costs. The NCCI data shows that TBI-related medical payments represent about 5 percent of all lost-time medical payments, despite TBIs accounting for only 2.5 percent of lost-time claims, indicating their disproportionate expense.
Concussions Require Immediate Medical Evaluation
Concussions appear minor but carry serious consequences if mishandled. A worker struck by a falling object or experiencing a moderate fall may initially seem fine, yet develop cognitive problems, balance issues, or persistent headaches within days or weeks. Many workers fail to seek medical evaluation immediately after a head injury, thinking symptoms will resolve on their own. This delays documentation and complicates your workers compensation claim later. The first week after injury is critical because outpatient costs are heavily influenced by CT scans of the head and brain, which serve as baseline documentation for your claim. Physical therapy emerges as the top paid physician service for head injuries, accounting for substantial portions of outpatient costs. Proper early diagnosis and documentation of even mild concussions protects your claim eligibility and allows medical providers to track your actual recovery trajectory rather than guessing based on incomplete information.
Penetrating Injuries Demand Emergency Response
Penetrating head injuries from objects like metal fragments, broken glass, or tools represent a smaller percentage of workplace head injuries but carry extreme severity. These injuries require emergency medical response and typically result in immediate hospitalization. The medical response is straightforward: these cases demand emergency care without delay. What complicates these claims is the documentation burden. You need clear evidence of how the object entered the workplace, why safety protocols failed, and how the injury occurred during work duties. These cases require meticulous gathering of incident reports, witness statements, and photographic evidence of the scene, as insurers scrutinize penetrating injuries more heavily than other head injury types.
Understanding how these injuries occur and what makes them expensive sets the stage for navigating your claim. Your next step involves learning what rights you hold after a workplace head injury and how to file a claim with the Ohio Bureau of Workers’ Compensation.
Securing Your Claim After a Head Injury
Act Quickly to Report Your Injury
The moment you suffer a head injury at work, your focus shifts to two critical tasks: getting medical care and protecting your claim. Ohio’s workers compensation system requires you to act within specific timeframes, and missing deadlines costs you benefits. You must report your injury in writing to your employer within 30 days, though reporting immediately proves far smarter because it creates a clear record of when the injury occurred and prevents disputes later. Your employer then becomes obligated to provide you with a DWC-1 form, which officially starts your claim with the Ohio Bureau of Workers’ Compensation. Do not rely on verbal reports or casual mentions to coworkers. Write a formal email or letter to your supervisor and HR department documenting the date, time, location, what caused the injury, and which body parts were affected. Keep a copy for yourself. This written record becomes invaluable if your claim faces scrutiny or denial later.

Build Your Medical Documentation Foundation
Medical documentation forms the backbone of every successful head injury claim in Ohio. After your initial emergency care, you need comprehensive baseline testing within the first week because outpatient costs are heavily driven by CT scans of the head and brain, which establish what your injury actually looks like. Request copies of all medical records, imaging results, and physician notes immediately after each appointment. Track every expense related to your injury: co-payments, travel costs to appointments, prescription receipts, and even parking fees. The NCCI data shows that physical therapy becomes the top paid physician service for head injuries, so expect this to be a major component of your recovery plan. If your doctor refers you to a neurologist, neuropsychologist, or physical therapist, accept those referrals promptly because these specialists document the severity and functional impact of your injury in ways that strengthen your claim.
Understand Your Eligibility and Coverage
Any head injury occurring during work duties qualifies for coverage under Ohio law, regardless of whether fault is clear. The injury can result from a single accident or repeated exposure, and workers compensation covers the full range of necessary medical care including tests, medications, equipment, and travel expenses to medical appointments. Your benefits include medical treatment, temporary disability payments while you cannot work, and permanent disability benefits if you reach a point where your condition stabilizes but you have lasting limitations. The permanent disability rating assigned at your maximum medical improvement point determines long-term benefits, so the thoroughness of your medical documentation directly influences that rating. If you reach maximum medical improvement but cannot return to your previous job, Ohio law may provide supplemental job displacement benefits to fund retraining or career transition services.
Know Your Wage Replacement and Settlement Rights
Most workers receive approximately two-thirds of their average weekly wages as temporary disability benefits, though the exact percentage depends on your specific circumstances and Ohio’s current wage replacement formulas. Do not accept any settlement offer without consulting a workers compensation attorney first, particularly for moderate to severe head injuries. Insurers often make early settlement offers that undervalue long-term medical needs and future earning capacity. Once you sign a settlement agreement, your claim closes and further payments for that injury stop, making it impossible to recover additional compensation if your condition worsens or unforeseen complications emerge. The next section addresses the obstacles that commonly arise during head injury claims and how to overcome them.
Common Challenges in Head Injury Claims
Insurers scrutinize head injury claims far more heavily than other workplace injuries because the medical costs and long-term care requirements drive significantly higher payouts. The National Council on Compensation Insurance found that while traumatic brain injuries account for only 2.5 percent of lost-time claims, they consume 5 percent of all lost-time medical payments-and roughly 2.5 percent of TBI claims exceed six figures, with these high-cost cases accounting for more than half of all TBI total incurred costs. This financial reality means insurance companies deploy aggressive tactics to minimize what they pay, and you face three primary obstacles that derail most unrepresented workers: proving your injury actually happened at work, overcoming claim denials or endless delays, and documenting long-term effects that justify ongoing treatment.
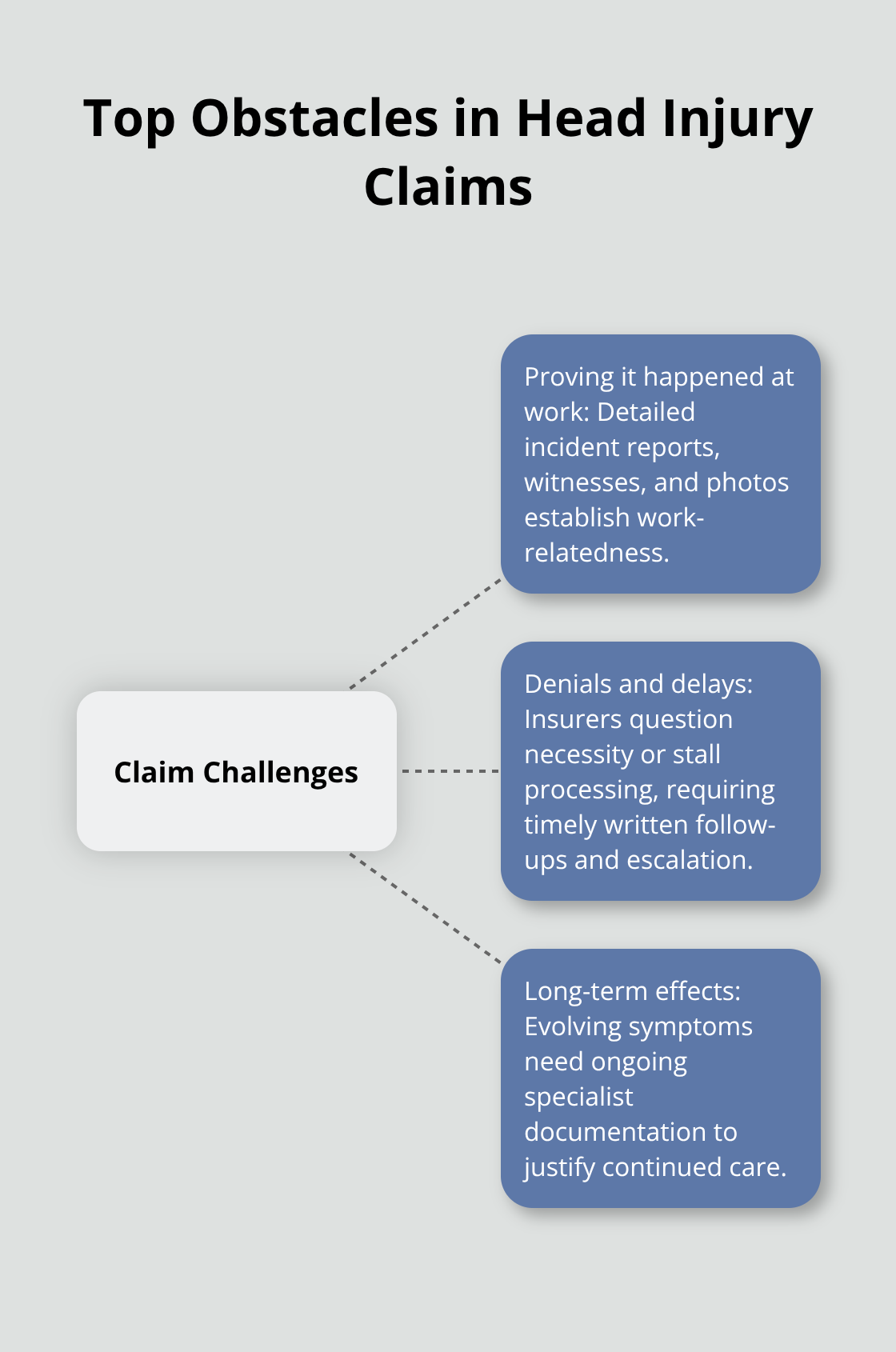
Establishing Your Injury Occurred at Work
Insurance companies demand concrete proof that your head injury happened during work duties, not before or after your shift. This sounds straightforward but becomes complicated when you cannot identify a specific witness or when the injury resulted from a routine task that went wrong unexpectedly. Your written incident report matters enormously here-the one you filed with your employer within 30 days. If that report contains vague language like “fell down” or “hit my head,” the insurer will argue the injury details remain unclear. Instead, your documentation must specify exactly what you were doing, which equipment or surface involved contact, how the impact occurred, and whether other workers witnessed the event. Photograph the location where the injury happened if possible, showing equipment positioning, floor conditions, or hazards that contributed to the fall or impact. If witnesses exist, collect their names and contact information immediately because memory fades and workers move jobs. The medical records from your first appointment carry weight too-if you reported the injury to your doctor and explained it happened at work, that contemporaneous medical documentation supports your claim. Insurers cannot easily dismiss medical records created the day of injury because they constitute real-time reporting rather than reconstructed accounts months later.
Fighting Denials and Delays That Starve Your Claim
Claim denials arrive in multiple forms, and each requires different responses. Some insurers deny claims outright, claiming insufficient evidence of a work-related injury. Others approve initial claims but deny specific medical treatments, arguing the proposed therapy lacks medical necessity. Still others delay claim processing indefinitely, neither approving nor denying, which effectively cuts off your benefits while disputes drag on. The NCCI data reveals that medical payments for head injuries shift dramatically over time-early costs concentrate on facility and physician services, with hospital inpatient stays representing the largest facility expense, but after the first year, payments shift toward drugs and other medical services. This pattern matters because insurers sometimes deny year-two or year-three treatment requests by claiming your injury should have fully resolved by then, even though the data shows legitimate medical needs often extend well beyond the first year. If your claim faces denial, request the specific reason in writing and obtain copies of the medical records or reports the insurer relied upon when making that decision. Many denials rest on incomplete information or outdated medical opinions, and you can challenge them by submitting updated medical documentation from your treating providers. Delays are trickier because the insurer technically has not denied anything-they simply have not processed your request. Set a clear deadline in writing: request that the insurer approve or deny your claim within 14 days, and if they miss that deadline, escalate to the Ohio Bureau of Workers’ Compensation for intervention. Documentation of your repeated requests and the insurer’s failure to respond becomes critical evidence if your case requires further dispute resolution.
Managing Conditions That Evolve Beyond Initial Diagnosis
Head injuries frequently produce complications that emerge weeks or months after the initial injury, and your claim documentation must anticipate these developments. The NCCI data shows that post-year-one medical payments for head injuries often include anticonvulsants and psychotherapeutic medications, indicating that neurological and psychological complications frequently emerge after initial recovery appears underway. Some workers develop chronic headaches that persist for years, others experience cognitive difficulties that surface only when they attempt returning to work, and still others struggle with mood changes or anxiety that compound the physical injury. Your medical team must document these developments thoroughly and connect them causally to the original head injury. If your neurologist identifies post-traumatic headaches or your neuropsychologist documents persistent cognitive deficits, those reports become essential to your claim because they justify continued medical treatment and potential permanent disability benefits. Do not assume your workers compensation insurer will automatically approve ongoing treatment simply because you have an open claim-you may need to submit updated medical documentation quarterly or when new symptoms emerge to prevent treatment denials. The insurer’s position will be that you have reached maximum medical improvement and should not need further care, so your medical providers must actively document why treatment remains necessary and how it addresses documented deficits from your injury.
Final Thoughts
Your head injury workers compensation claim succeeds when you act decisively from the moment injury occurs. Report your injury in writing to your employer within 30 days, gather comprehensive medical documentation immediately, and refuse to accept any settlement offer without professional legal review. These three actions create the foundation that prevents insurers from denying your claim or undervaluing your benefits.
Legal representation transforms head injury claims fundamentally because insurers deploy experienced claims adjusters trained to minimize payouts while counting on injured workers to navigate the system alone. An attorney levels this imbalance by handling insurer communications, challenging denials with medical evidence, and negotiating settlements that account for future medical costs and earning capacity. Your permanent disability rating, determined at maximum medical improvement, shapes benefits for years or decades depending on your age and injury severity.
We at Robin J Peterson Company, LLC represent injured workers throughout Ohio, fighting against insurers to secure the benefits you deserve. If your claim faces denial, delay, or inadequate settlement offers, contact our team for a consultation. Your recovery depends on protecting your rights now, and that protection begins with experienced legal guidance tailored to your specific circumstances.
