If you’ve suffered a workplace injury in Ohio and had a previous condition, the Second Injury Fund details matter more than you might think. This fund can significantly change how your workers’ compensation claim plays out.
At Robin J Peterson Company, LLC, we’ve guided countless injured workers through the complexities of Second Injury Fund claims. Understanding how this fund works puts you in a stronger position to protect your benefits.
What the Ohio Second Injury Fund Actually Does
Ohio created the Second Injury Fund to solve a real employment problem: employers refused to hire workers with disabilities because they feared compounded liability if a new injury occurred. The state designed this fund to remove that disincentive by stepping in to cover the extra costs when a pre-existing condition combines with a new workplace injury to create substantially greater disability. This wasn’t theoretical policy-it was a direct response to employment discrimination against disabled workers. According to the Ohio Industrial Commission, the fund has contributed to roughly a 28% increase in employment opportunities for workers with disabilities since implementation, which demonstrates that removing employer fear actually changes hiring behavior.

How the Fund Covers Your Combined Disabilities
The Second Injury Fund operates within strict parameters. It covers three specific categories of expenses: medical costs tied to the enhanced disability, lost wage benefits, and vocational rehabilitation expenses. Critically, the fund only reimburses the portion of disability attributable to how the two conditions interact-not the entire disability from either condition alone. To qualify, you need a pre-existing permanent physical impairment rated at least 15% disability and a new workplace injury that, combined with the pre-existing condition, creates either 50% or more permanent partial disability or permanent total disability. The Ohio Industrial Commission processes these claims, and incomplete applications face automatic denial. This specificity matters because vague documentation about your pre-existing condition is the leading reason claims fail. According to Ohio Industrial Commission data, more than 60% of Second Injury Fund claims are rejected due to insufficient documentation linking the pre-existing condition to worsened outcomes.
Why Documentation Quality Determines Your Success
Your pre-existing condition must be permanent to qualify-temporary conditions don’t open eligibility. You’ll need baseline medical records from before your new injury, functional capacity evaluations that show how the combined conditions affect your work capacity, and multiple physician opinions that explain how the new injury worsened your pre-existing impairment. Claims supported by multiple medical opinions showing this causation connection are about 84% more likely to succeed than those with a single physician report. Start collecting these records immediately after your new injury occurs. The timeline matters too-appeals must be filed within 14 days of denial, and delays from incomplete submissions can average about 147 days. Represented claimants win about 78% of Second Injury Fund cases versus 23% for self-represented claimants, according to Ohio Industrial Commission data, which suggests the complexity of assembling proper evidence significantly impacts outcomes.
What Happens When You File Your Claim
The Ohio Industrial Commission requires specific forms and medical evidence that links your new injury to the increased impairment. Initial denials occur in about 67% of Second Injury Fund applications, but when properly represented, appeals succeed about 43% of the time. An experienced workers’ compensation attorney coordinates with treating physicians, independent specialists, and pre-injury records to build comprehensive documentation and support disability calculations. This legal coordination addresses the denial reasons directly and strengthens your appeal with objective evidence such as functional capacity evaluations and expert testimony. The representation advantage is substantial-your attorney maximizes overall benefits by calculating future medical costs, ongoing wage replacement, and vocational rehabilitation needs.
Who Qualifies for Second Injury Fund Benefits
Under Ohio law, a second injury isn’t simply any new workplace accident that happens after you’ve had a prior condition. The Second Injury Fund has strict eligibility rules that separate legitimate claims from those that don’t meet the legal threshold. You must have a pre-existing permanent physical impairment rated at least 15% disability according to the Ohio Industrial Commission guidelines. That pre-existing condition can stem from a work-related injury, a non-work illness, or even a congenital condition-the source doesn’t matter, only that it’s permanent and documented. Your new workplace injury must then combine with that pre-existing impairment to create substantially greater disability. Specifically, the combined effect must result in either 50% or more permanent partial disability or permanent total disability. This isn’t about adding percentages together informally; the Ohio Industrial Commission evaluates how the two conditions interact medically to produce the enhanced disability level.

The fund reimburses only the portion of disability attributable to that interaction, not the entire impairment from either condition alone. This distinction is critical because many workers and even some employers misunderstand it, assuming the fund covers the full scope of the new injury.
What Medical Evidence the Ohio Industrial Commission Requires
The documentation requirement is where most claims fail. You need to start with your pre-injury medical records-baseline imaging, physician notes, and any disability ratings assigned before your new injury. Then obtain functional capacity evaluations conducted after your new injury that specifically compare your work capacity before and after the combined conditions took effect. Independent medical examinations from physicians not treating you directly carry substantial weight because they appear unbiased to the Ohio Industrial Commission. Multiple physician opinions explaining the causal link between your new injury and the worsened pre-existing condition are essential; according to the Ohio Industrial Commission, claims with multiple supportive medical opinions succeed about 84% more often than those relying on a single physician report.
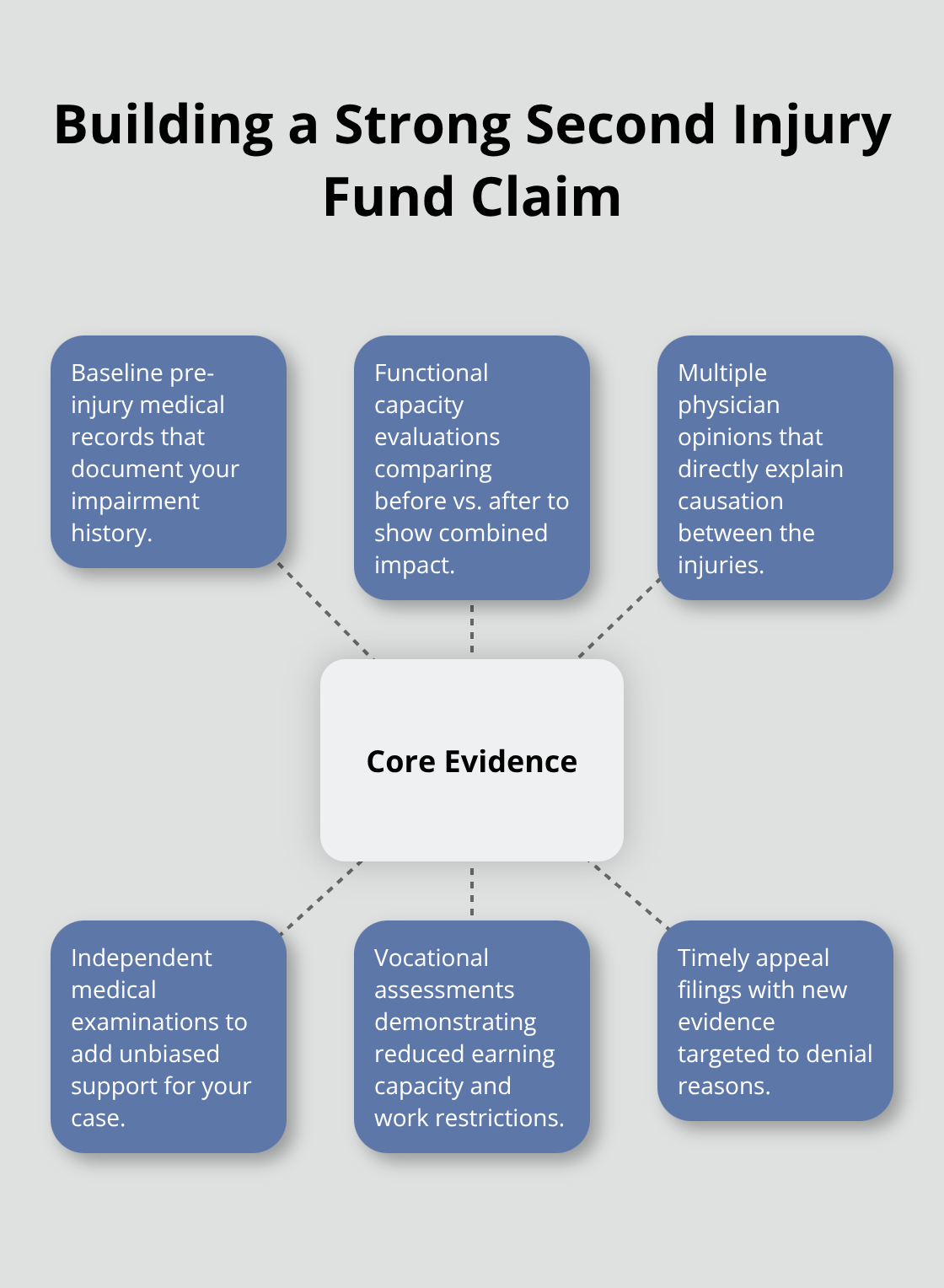
How to Document the Interaction Between Your Two Conditions
Vague statements that you’re worse off won’t survive review. You need specific documentation of how the new injury prevented the pre-existing condition from stabilizing or how it created new functional limitations beyond what the pre-existing condition alone would cause. Vocational assessments that detail your reduced earning capacity and work restrictions (given the combined conditions) also strengthen your claim significantly. These assessments show the Ohio Industrial Commission exactly how your combined disabilities affect your ability to work and earn income.
The Critical 14-Day Appeal Deadline
The 14-day appeal deadline is absolute-missing it bars your claim from reconsideration. Mark this date immediately after you receive any denial notice from the Ohio Industrial Commission. Delays from incomplete submissions can average about 147 days, so acting quickly with complete documentation prevents unnecessary waiting periods. When you file your appeal, new medical evidence or expert testimony addressing the specific denial reasons typically determines whether the Ohio Industrial Commission reverses its initial decision.
How the Second Injury Fund Changes Your Claim Outcome
The Second Injury Fund fundamentally alters how your workers’ compensation claim operates by shifting a portion of your long-term liability away from your employer’s insurer to the state fund. When the Ohio Industrial Commission approves your Second Injury Fund claim, the fund becomes responsible for covering the specific portion of your disability that results from the interaction between your pre-existing condition and your new workplace injury. This matters directly to your benefits because it determines which entity pays your medical expenses, wage replacement, and vocational rehabilitation costs.
What the Fund Actually Covers
The fund covers three distinct categories: medical expenses tied specifically to the enhanced disability, lost wage benefits attributable to the combined effect, and vocational rehabilitation costs necessary because of the compounded disability. Your employer’s insurer typically pays benefits first, and the Second Injury Fund then reimburses the portion attributable to how your conditions interact. This sequence affects the timing and amount of your benefits because the fund only activates after the initial claim determination. The Ohio Industrial Commission calculates this interaction carefully-they don’t simply subtract your pre-existing disability percentage from your combined disability and call that the fund’s portion. Instead, they examine medical evidence showing exactly how your new injury prevented stabilization of your pre-existing condition or created additional functional limitations beyond what either condition would cause independently.
How Medical Evidence Shapes Your Benefit Calculation
Your physician’s specific testimony about causation matters tremendously to the actual benefit calculation. The Ohio Industrial Commission requires objective proof that the new injury worsened your pre-existing condition in measurable ways. This medical-legal analysis separates successful claims from those that fail due to insufficient documentation. Legal representation fundamentally changes your outcome-represented claimants win approximately 78% of cases compared to 23% for self-represented workers. Your treating physicians, independent medical specialists, and vocational experts all contribute evidence that the Ohio Industrial Commission weighs when determining the fund’s liability.
Why Your Claim Structure Extends Beyond Standard Workers’ Compensation
Your claim structure changes significantly under Second Injury Fund involvement because future medical costs, ongoing wage replacement, and vocational rehabilitation expenses may extend far longer than they would under standard workers’ compensation alone. The fund remains liable for any remaining benefits after your employer’s insurer obligations end, which provides a safety net for long-term disability support. This extended timeline means you need comprehensive documentation of your future medical needs and reduced earning capacity over time. Inadequate documentation results in the fund covering only partial medical costs when comprehensive vocational assessments would have secured coverage for rehabilitation expenses as well.
The Documentation Coordination That Strengthens Your Claim
The initial denial rate of about 67% according to Ohio Industrial Commission data reflects how frequently claims lack coordinated evidence presentation. Coordination with treating physicians, independent medical specialists, and vocational experts ensures the Ohio Industrial Commission receives objective evidence supporting the full extent of your enhanced disability. We at Robin J Peterson Company, LLC focus on calculating the full scope of your future medical needs and structuring your claim to maximize what the Second Injury Fund covers rather than what your employer’s insurer pays. This approach directly addresses the common deficiencies that lead to denials before submission or on appeal.
Final Thoughts
The Second Injury Fund details reveal a system that protects workers when a new injury compounds an existing condition, and understanding how this fund operates transforms your approach to your workers’ compensation claim. Initial denials occur in roughly 67% of applications, yet appeals succeed about 43% of the time when you present new medical evidence or expert testimony addressing the specific denial reasons. This gap between initial rejection and successful appeal demonstrates that documentation quality and legal strategy determine your outcome far more than the strength of your underlying claim.
Professional legal representation matters substantially because the complexity of coordinating medical evidence, meeting the critical 14-day appeal deadline, and calculating benefit interactions exceeds what most injured workers can manage alone. Represented claimants win approximately 78% of cases compared to 23% for self-represented workers according to Ohio Industrial Commission data. Your attorney coordinates with treating physicians, independent medical specialists, and vocational experts to assemble the objective evidence the Ohio Industrial Commission requires.
If you’ve suffered a new workplace injury and have a pre-existing permanent impairment, contact Robin J Peterson Company, LLC to evaluate whether the Second Injury Fund applies to your situation. The firm represents injured workers throughout Ohio’s Cleveland, Akron, and Canton metropolitan areas and focuses specifically on navigating the Ohio Bureau of Workers’ Compensation and Industrial Commission of Ohio. Your next step is gathering your pre-injury medical records and documenting your new injury immediately, then consulting with an experienced workers’ compensation attorney who understands how to maximize Second Injury Fund benefits.
