A workplace injury in Ohio can feel overwhelming, especially when you’re navigating the Bureau of Workers’ Compensation system for the first time. At Robin J Peterson Company, LLC, we’ve seen firsthand how quickly claims get denied or delayed when workers don’t have the right Ohio workers comp resources at their fingertips.
This guide walks you through the essential tools, deadlines, and common pitfalls that affect your claim. The right information now can make the difference between a smooth process and months of frustration.
How Ohio’s Workers Comp System Actually Works
Filing a workers compensation claim in Ohio requires you to understand the state’s strict timeline and specific procedures. The Bureau of Workers’ Compensation operates under a no-fault system, meaning you don’t need to prove your employer was negligent to receive benefits-you only need to show the injury occurred during employment. The critical first step is reporting your injury to your employer in writing as soon as it happens. Verbal reports create confusion and give employers wiggle room to claim they never received notice.
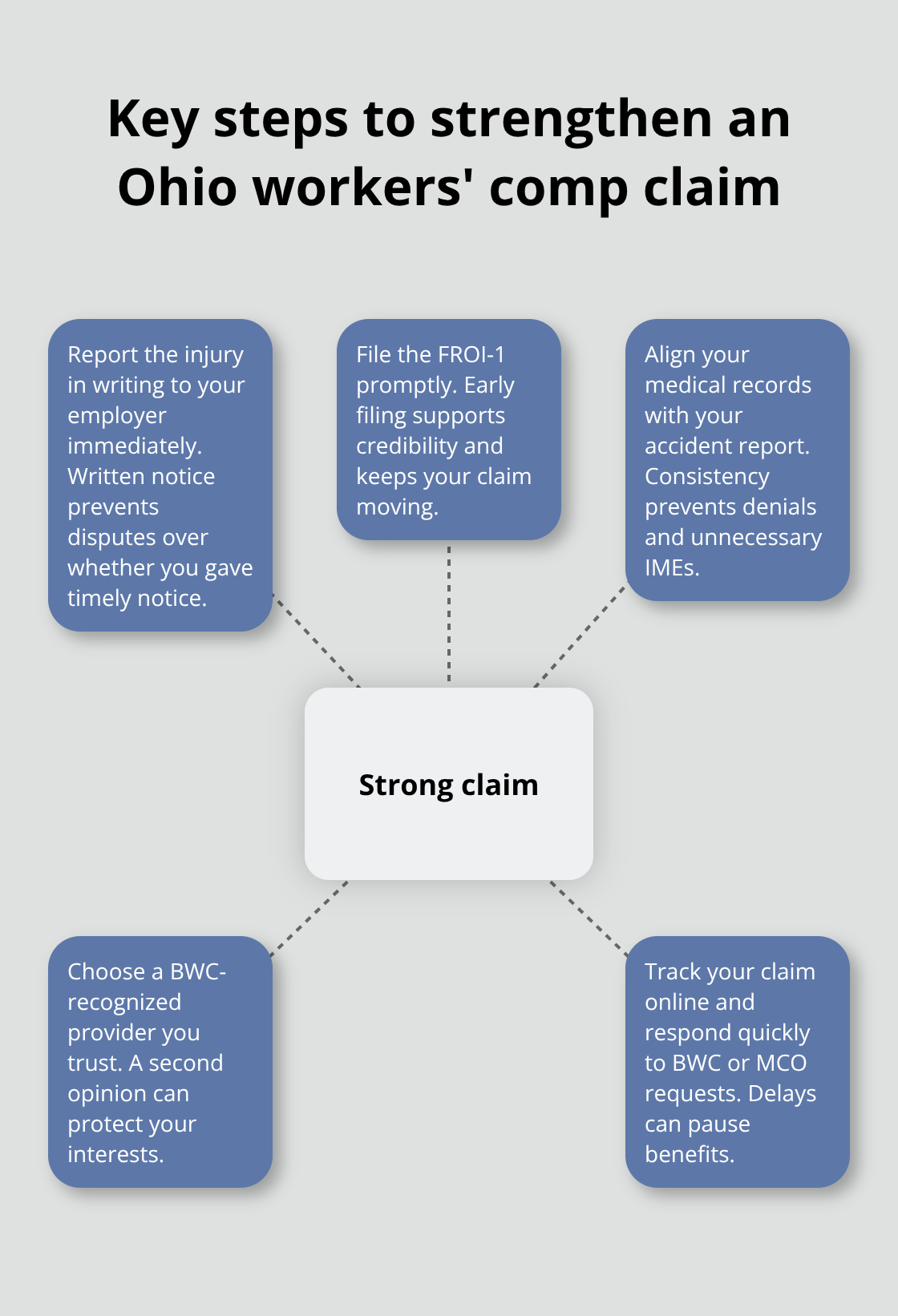
File the First Report of Injury Immediately
After you notify your employer, you or your medical provider must file the First Report of Injury (the FROI-1) with the BWC. This form can be submitted online, by mail, or by phone, and it must include the exact date, time, and nature of your injury. Ohio law gives you one year from the injury date to file, but delays significantly weaken your claim’s credibility with the BWC and any investigating medical professionals. Waiting to file the FROI-1 ranks among the biggest mistakes workers make-the sooner you submit it, the stronger your position becomes.
Match Your Medical Records to Your Accident Report
Accuracy in your initial accident report directly determines whether your claim moves forward or gets rejected. The medical records from your first treatment must match your accident report exactly. If you tell your employer you injured your back lifting boxes but later tell a doctor you were reaching for something on a shelf, that inconsistency becomes ammunition for denial. Be specific and honest about what happened, including any pre-existing conditions that might have contributed to the injury.
Medical providers and managed care organizations scrutinize these details, and contradictions can trigger independent medical examinations that often work against claimants. Create a written paper trail immediately-send emails to your employer confirming the injury details, keep copies of all accident reports, and maintain records of every communication with your employer, the BWC, and your healthcare provider. This documentation becomes essential if your claim faces a dispute or denial.
Choose Your Medical Provider Strategically
Once the FROI-1 reaches the BWC, a managed care organization coordinates your medical treatment and claim processing. You can receive treatment from any doctor recognized by the Bureau of Workers’ Compensation-you’re not limited to your employer’s choice, though many workers incorrectly assume they are. If your employer directed you to a specific physician, a second opinion from a doctor of your choosing protects your interests and ensures independent medical assessment.
Track Your Claim Status and Respond Promptly
The BWC typically processes claims within ten business days, but this assumes your documentation is complete and accurate. After approval, your MCO assigns you a case manager who handles medical authorizations and benefit payments. You can track your claim status regularly through the BWC’s online portal using the View My Claim feature, and you must respond promptly to any communications from the BWC or your MCO. Delays in responding to requests can halt your benefits and create gaps in coverage that become difficult to recover.
Understanding these steps positions you to move forward with confidence, but the real challenge emerges when complications arise-which is why knowing what resources exist and when to access them separates workers who protect their benefits from those who lose them.
Where to Find Help When Your Claim Stalls
The BWC Help Center and Official Resources
The BWC operates a Help Center that functions as your primary starting point for navigating the system, offering step-by-step guidance, forms, and frequently asked questions covering every stage of the claims process. You can access this resource online without appointment or cost, and it answers specific questions about filing deadlines, documentation requirements, and benefit eligibility. Beyond the Help Center, the Ohio Industrial Commission and its independent Ombuds Office exist specifically to resolve disputes and provide support when claims face denial or delay.
The Ombuds Office: Your Independent Advocate
The Ombuds Office operates separately from the BWC itself, meaning an investigator can examine your case objectively and push back against bureaucratic obstacles that block legitimate claims. When you contact the Ombuds Office, provide them with copies of your FROI-1, medical records, and any denial letters you’ve received-this documentation allows them to identify exactly where your claim derailed. The BWC also maintains service offices across Ohio at physical locations where staff can review your claim in person, which proves valuable when written communications haven’t resolved your issues.

The main office sits at 30 W. Spring St., Columbus, OH 43215-2256, and you can locate your nearest service office through the BWC website to access face-to-face assistance. If your claim stalls beyond 30 days, contact the Ohio Bureau of Workers’ Compensation directly at this location.
When You Need Legal Representation
An experienced workers’ compensation attorney becomes essential when claims face denial, when settlement offers arrive before your condition stabilizes, or when the MCO creates obstacles to necessary medical treatment. Many workers delay hiring an attorney hoping to manage the process independently, but this hesitation costs them thousands in missed benefits and rejected claims. An attorney who specializes in Ohio workers’ compensation understands how to interpret MCO communications, prepare you for independent medical examinations, and file appeals that actually succeed-skills that generic legal services simply cannot provide.
Legal representation becomes especially critical if you’re considering a settlement, since accepting a final payment without understanding your long-term medical needs or how your injury affects future earning capacity can permanently eliminate access to ongoing treatment and wage replacement benefits. The decision to hire an attorney should not wait until your claim faces outright denial; early intervention prevents problems from escalating and protects your position throughout the entire process.
What Mistakes Actually Sink Ohio Workers Comp Claims
The One-Year Filing Deadline Is Absolute
The one-year filing deadline for Ohio workers compensation claims sounds straightforward until injured workers miss it constantly, and the consequences are permanent. The Bureau of Workers’ Compensation enforces this deadline strictly-file after twelve months from your injury date and your claim gets rejected outright, regardless of how legitimate your injury is. The clock starts the moment the injury occurs, not when you report it to your employer or seek medical treatment. If you injured yourself on January 15th and didn’t file your FROI-1 until January 20th of the following year, that claim dies.

Exceptions exist for certain chronic occupational illnesses where exposure happened over time, but these narrow circumstances don’t apply to acute injuries from falls, equipment accidents, or sudden trauma.
Don’t assume your employer will file the FROI-1 correctly or on time. Taking responsibility for filing yourself eliminates the risk that bureaucratic delays or employer negligence destroy your eligibility. Many workers wait six months thinking they have plenty of time, only to discover they’ve already burned through half their window.
Inconsistencies Between Reports and Medical Records Trigger Denials
Inconsistencies between your accident report and medical records create the second major vulnerability that triggers denials and investigations. Workers tell their employer one version of what happened, then tell a doctor something slightly different, and the managed care organization uses that contradiction as justification for denial or demanding an independent medical examination that often contradicts your account. The specifics matter tremendously-if you reported lifting boxes but later mention you were reaching overhead, the MCO interprets this as either deception or memory problems that undermine your credibility.
Medical providers also make documentation errors. They might record an incomplete injury description or fail to link your treatment directly to the workplace incident, which then gives the BWC grounds to question whether the injury actually qualifies for coverage. You must review your medical records against your initial accident report and correct any discrepancies immediately, before they harden into official documentation that contradicts your claim.
Documentation Gaps Create Permanent Vulnerabilities
Documentation gaps compound credibility problems significantly. Workers who fail to report injuries in writing, who rely on verbal conversations with supervisors, or who don’t preserve emails and written communications create situations where the employer later claims no notice ever arrived. A single email to your supervisor (sent immediately after the injury) documents the exact time it occurred and the specific activity involved-this becomes invaluable evidence if disputes emerge later.
Create a written paper trail from day one. Send emails to your employer confirming the injury details, keep copies of all accident reports, and maintain records of every communication with your employer, the BWC, and your healthcare provider. This documentation becomes essential if your claim faces a dispute or denial, and it protects your position when the MCO questions whether your injury actually happened as you described it.
Final Thoughts
The Ohio workers comp resources available through the Bureau of Workers’ Compensation and the Industrial Commission exist specifically to protect injured workers who access them strategically. Your immediate actions matter most: report your injury to your employer in writing, file your FROI-1 within days rather than weeks, and create a documented paper trail of every communication related to your claim. These steps cost nothing and take minimal time, yet they eliminate the most common vulnerabilities that sink legitimate claims.
When complications arise, the BWC Help Center and Ombuds Office provide free resources that many workers never discover. The Ombuds Office operates independently from the BWC itself, meaning investigators can push back against bureaucratic obstacles and examine your case objectively. Service offices across Ohio also offer in-person assistance when written communications haven’t resolved your issues, and an experienced workers’ compensation attorney interprets MCO communications, prepares you for independent medical examinations, and files appeals that succeed.
The most critical decision you’ll make involves hiring legal representation before you accept any settlement offer, since finalizing a settlement without understanding your long-term medical needs can permanently eliminate access to ongoing treatment. Contact our firm to discuss how we can protect your claim and guide you through the complexities of Ohio’s workers’ compensation system.
