Filing a workers’ compensation claim in Ohio can feel overwhelming if you don’t know where to start. We at Robin J Peterson Company, LLC help injured workers navigate the BWC claim filing basics every day.
This guide walks you through the process step-by-step, from reporting your injury to submitting your claim and avoiding common mistakes that delay approvals.
How the Ohio BWC Works and Why Speed Matters
The No-Fault System Sets BWC Claims Apart
The Ohio Bureau of Workers’ Compensation operates as a state agency that manages workplace injury claims across the state. Unlike private insurance, the BWC is a government-run system where your employer pays into a fund that covers medical treatment, wage replacement, and rehabilitation services for injured workers. The BWC does not determine fault the way a lawsuit would.
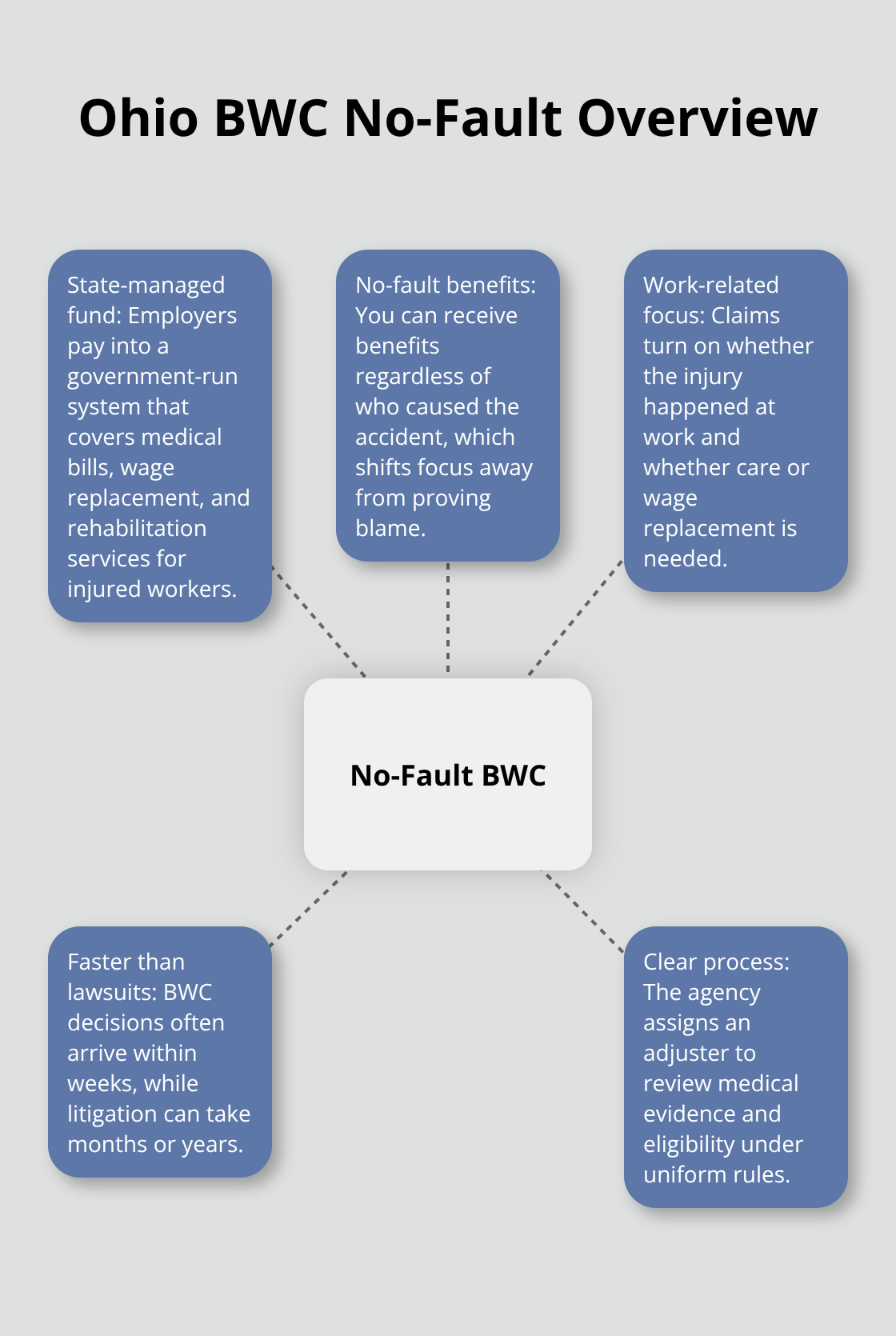
Instead, it follows a no-fault system, meaning you can receive benefits regardless of who caused the accident. This distinction matters significantly because it changes how your claim moves through the system.
A BWC claim focuses on whether your injury happened at work and whether you need medical care or lost wages. A lawsuit, by contrast, requires proving negligence or wrongdoing, which takes longer and involves different legal standards. Most injured workers in Ohio benefit from the speed of the BWC system rather than pursuing a lawsuit, since BWC claims typically generate decisions within weeks, while litigation can stretch across months or years.
Strict Deadlines Control Your Access to Benefits
Filing deadlines in Ohio are strict and unforgiving. You must report your injury to your employer within one day of the incident, according to Ohio Administrative Code 4121-3-01. Your employer then has ten days to file the claim with the BWC. Missing these windows closes your access to benefits, and the BWC will not extend deadlines for missed paperwork or late submissions.
Once your employer reports the injury, the BWC assigns a claims adjuster who reviews medical evidence and determines eligibility. Initial claim decisions typically arrive within two weeks, though complex cases may take longer. The sooner you report and the more thorough your initial paperwork, the faster your benefits start flowing.
Documentation Drives Claim Speed and Approval
You must document everything from day one, including the exact time and location of the injury, witness names, and any equipment involved. Keep medical appointments, follow your doctor’s treatment plan, and maintain records of all prescriptions and restrictions. The BWC reviews these materials to make decisions, so incomplete or delayed documentation directly slows your claim’s progress. Workers who maintain comprehensive records (medical visits, test results, and work restrictions) move through the system faster than those who submit scattered paperwork months after their injury.
Now that you understand how the BWC system operates and why speed matters, the next step involves taking action immediately after your injury occurs.
Filing Your Injury Report and Getting Your Claim Moving
Report your injury to your employer on the same day it happens. The Ohio Administrative Code requires this, and waiting even a few hours creates friction that slows everything down. Do not assume your supervisor will handle it or that you can file later. Written notification matters more than verbal reports because written records establish the official timeline and protect you if questions arise later. Email your employer a simple message stating the date, time, location, what happened, and which body part was injured. Keep a copy for yourself. This single action prevents disputes about when your employer learned of the injury and forces the claim process to start immediately.
Your employer must submit the claim to the BWC within ten days of learning about your injury. While your employer handles the filing, you control the speed of medical care by seeking treatment promptly. Do not delay visiting a doctor to wait for the claim to be approved. Get medical attention immediately after the injury, even if you think it is minor. Medical records created on or near the injury date carry far more weight than records created weeks later. The BWC uses these early medical documents to decide whether your injury is work-related and whether you qualify for benefits. Gather the name and contact information of your treating physician, the exact diagnosis, any prescribed medications, and any work restrictions before the claim is filed. Having this information ready means your employer can include it in the initial filing, which accelerates the BWC’s review.
Organize Your Documentation Before Submitting
Collect everything related to your injury before your employer files with the BWC. Take photographs of the equipment, work area, or condition that caused the injury if safely possible. Write down the names and contact information of anyone who witnessed the accident. If a police report was filed, obtain a copy. Medical records should include your initial visit notes, test results, imaging reports, and any follow-up appointments. Store these documents in a cloud-based system with automatic backups so you cannot lose them if your computer fails. The BWC adjuster will request these materials multiple times throughout your claim, and having them organized saves weeks of back-and-forth communication. Workers who arrive with complete documentation move through decisions 30 to 40 percent faster than those who scramble to find records later.
Submit Accurately and Track Your Claim Number
Your employer submits the claim through the Ohio BWC online portal or via authorized third-party administrators. The BWC then assigns a claim number and identifies a claims adjuster. Request this claim number immediately after submission and save it. Use the number to check your claim status through the BWC’s online system, which shows whether the adjuster has received medical records, what stage your claim occupies, and when decisions are expected. Many injured workers ignore their claim number and lose track of progress, which leads to missed deadlines and forgotten follow-ups. Set a calendar reminder to check your claim status every two weeks. If the adjuster requests additional information, respond within three days rather than waiting a week. Speed in responding to information requests directly shortens the time until your benefits begin.

What Happens Next in the Claims Process
Once you submit your claim with complete documentation and a clear claim number, the BWC adjuster enters the review phase. The adjuster examines your medical records, witness statements, and incident details to determine whether your injury qualifies for benefits. This stage moves faster when you have already provided thorough documentation and respond quickly to any requests for clarification. Understanding your legal rights after job injury helps you navigate this critical phase with confidence. The next chapter covers the mistakes that slow or derail claims at this critical juncture, and how to avoid them.
What Derails BWC Claims Most Often
The gap between filing a claim and receiving a decision is where most injured workers stumble. Three specific mistakes account for the majority of delays and denials. The first mistake is misunderstanding Ohio’s reporting timeline. You have one day to notify your employer, and your employer has ten days to file with the BWC. Many workers assume they can report an injury after a week or two, especially if symptoms develop slowly. This assumption costs you. The Ohio Administrative Code is explicit: late reporting triggers investigation delays and can result in the BWC questioning whether your injury truly happened at work. Claims get delayed by six to eight weeks when a worker waits four days to report a shoulder strain that worsened gradually. The second mistake is submitting incomplete forms or omitting critical details. The BWC adjuster needs your exact injury time, location, witness names, medical provider contact information, and a clear description of how the injury occurred. Missing any of these elements forces the adjuster to contact you for clarification, which adds two to three weeks to processing time. Workers often leave sections blank thinking they can fill them in later, but the BWC does not work that way. Incomplete initial submissions move to the back of the queue while the adjuster waits for your response.
The Cost of Silence After Filing
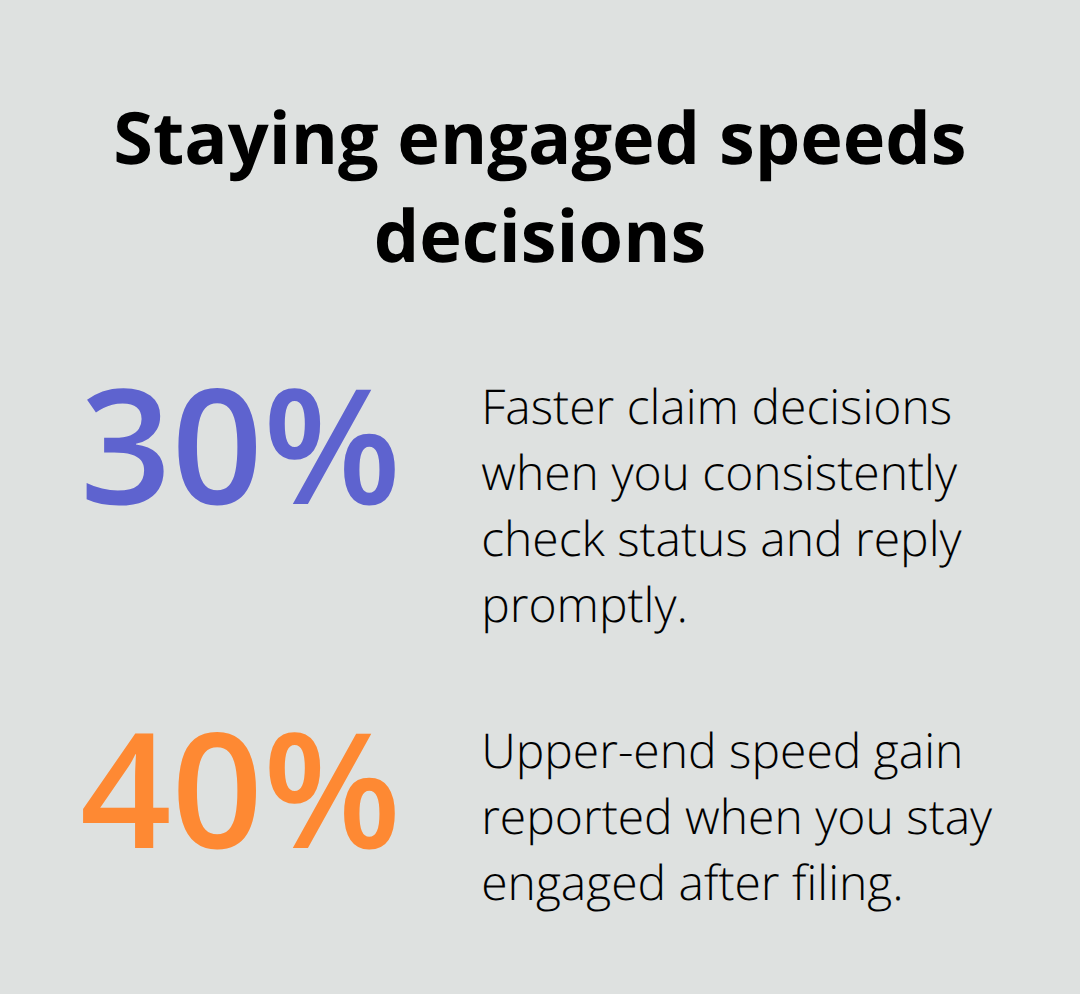
The third mistake is vanishing after you submit your claim. Many injured workers file their paperwork and assume the process moves forward automatically. In reality, the adjuster needs your cooperation throughout the review. Medical providers sometimes delay sending records. Insurance companies request additional documentation. The adjuster may need you to clarify what happened at the moment of injury. If you do not respond within three to five days, your claim stalls. Workers who check their claim status every two weeks and respond immediately to adjuster requests move through decisions 30 to 40 percent faster than those who go silent after filing.
Build a System That Prevents Delays
The practical solution to all three mistakes is establishing a simple system on day one. Write down your injury date and time immediately, including the exact location and what you were doing. Email this information to your employer the same day and keep a copy. Within 24 hours, schedule a medical appointment and request that the provider send records directly to the BWC using your claim number once it is assigned. Create a folder (physical or digital) where you store your claim number, adjuster name, adjuster phone number, and all medical records. Set phone reminders on your calendar to check your claim status every two weeks using the BWC portal. When the adjuster contacts you requesting information, respond within two business days, not two weeks. This structure prevents the delays that plague most claims.
Why Consistency Matters More Than Perfection
The difference between a claim that moves quickly and one that stalls for months often comes down to whether you treat the process as a one-time filing or as an ongoing responsibility that requires consistent attention. Speed in responding to information requests directly shortens the time until your benefits begin. The adjuster reviews your medical records, witness statements, and incident details to determine whether your injury qualifies for benefits. This stage moves faster when you have already provided thorough documentation and respond quickly to any requests for clarification.
Final Thoughts
Filing a BWC claim in Ohio requires speed, accuracy, and follow-through from the moment your injury occurs. The BWC claim filing basics boil down to three actions: report your injury to your employer within one day, gather complete documentation immediately, and respond promptly to every request from your claims adjuster. Workers who treat their claim as an active responsibility rather than a one-time filing move through the system faster and receive benefits sooner.
Many injured workers navigate this process successfully on their own, but complex cases, denied claims, or disputes with the BWC benefit from professional guidance. Missing a deadline or submitting incomplete paperwork can cost you access to medical care and wage replacement benefits. An attorney who understands Ohio workers’ compensation law can review your claim, identify potential problems before they delay your benefits, and represent you if the BWC denies your claim.
Contact Robin J Peterson Company, LLC if your claim has been delayed, denied, or if you need guidance navigating the appeals process. Stay engaged after you submit your claim by checking your status every two weeks, responding quickly to adjuster requests, and maintaining detailed records of all communications. Your claim is not complete until you receive your decision and your benefits begin flowing.
