Work injuries in Ohio can leave you confused about what benefits you’re actually entitled to. The Ohio Bureau of Workers’ Compensation handles most claims, but that’s far from your only option.
At Robin J Peterson Company, LLC, we know that injury compensation alternatives in Ohio extend well beyond traditional workers’ comp. This guide walks you through every pathway available to you.
How Ohio’s Injury Compensation System Actually Works
The MCO Structure That Controls Your Claim
The Ohio Bureau of Workers’ Compensation processes roughly 300,000 claims annually, making it the primary payer for work-related injuries in the state. Most injured workers don’t realize the system operates through a mandatory choice requirement that directly affects their medical care and claims speed. When you suffer a work injury in Ohio, your employer must select a Managed Care Organization (MCO) within 30 days of receiving their Certificate of Coverage, or the BWC assigns one automatically. This MCO becomes your gateway to everything: claim filing, medical treatment authorization, and benefit decisions. The MCO coordinates between you, your healthcare providers, your employer, and the BWC itself.
If your employer missed the 30-day window, this fact strengthens your position because it means the assigned MCO may not have been your employer’s preferred choice. The BWC also allows employers to work with Third-Party Administrators (TPAs) for cost management through programs like Group Rating and Group Retrospective Rating, but TPAs operate separately from medical management and don’t replace the MCO’s role. Your claim’s speed and quality depend heavily on which MCO handles your case. Open enrollment for MCO selection happens roughly every two years, meaning your employer could switch providers, which is why staying informed about who manages your claim prevents communication gaps.
Understanding Your Benefit Categories
Ohio offers multiple benefit categories that most injured workers confuse or overlook entirely. Temporary Total Disability (TTD) replaces 72 percent of your average weekly wage for the first 12 weeks if you cannot work at all, then drops to 66⅔ percent after that point. TTD requires you to miss at least seven consecutive days and reach a threshold where a doctor certifies you cannot perform any job, not just your old position.
Permanent Partial Disability (PPD) compensates you for permanent impairment even if you return to work, while Permanent Total Disability (PTD) applies when you cannot work in any capacity long-term. Temporary Partial Disability (TPD) covers situations where you can perform light-duty work but earn less than before your injury. The distinction between these categories directly impacts your financial recovery, yet many workers accept whatever the MCO initially offers without understanding they might qualify for higher-tier benefits.
Filing Your Claim Within Critical Deadlines
Filing a First Report of Injury (FROI) within one year of your injury protects your eligibility, though acting faster-ideally within 30 days-strengthens your claim significantly because early reporting prevents disputes over causation and timing. The speed at which you file your claim determines whether the MCO questions the work-relatedness of your injury or accepts it without challenge. Workers who wait months to report injuries often face additional scrutiny and longer processing times. Your employer and the MCO both benefit from quick reporting, which means you should contact your supervisor immediately after any workplace incident, even if you feel fine initially.
Beyond Workers’ Compensation
Social Security Disability Insurance as a Parallel Path
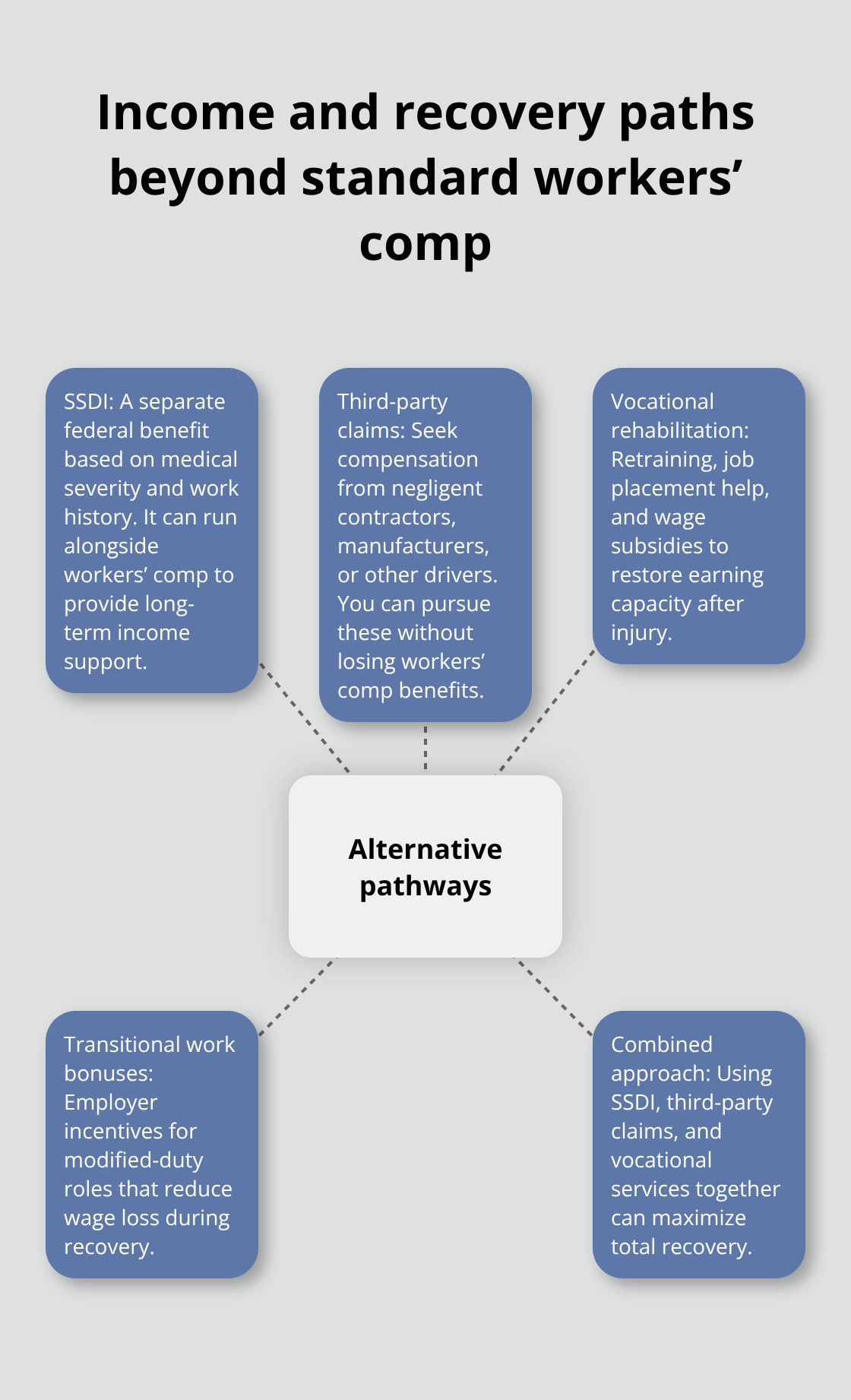
Social Security Disability Insurance offers a separate route when work injuries prevent you from earning income long-term, and the approval criteria differ significantly from Ohio workers’ comp requirements. The Social Security Administration approves SSDI based on medical severity and work history, not causation like the BWC does, which means you can qualify for SSDI even if your workers’ comp claim faces disputes. You must have paid into Social Security through payroll taxes and be unable to work for at least 12 months or face a terminal condition. The SSA processes SSDI applications slowly-initial decisions typically take three to six months, with many claims rejected on first submission. Roughly 70 percent of initial SSDI claims get rejected according to SSA data, but appeals reverse many of these rejections when proper medical documentation supports your case. The advantage here is that SSDI payments continue indefinitely if you qualify, unlike TTD which stops once you reach Maximum Medical Improvement. You can file for SSDI while your workers’ comp claim processes, meaning both systems can work simultaneously to support your recovery. This dual approach makes sense because workers’ comp covers immediate expenses while SSDI provides long-term security if your injury prevents return to any substantial work.
Third-Party Liability Claims Against Negligent Parties
Third-party liability claims exist when someone other than your employer caused your injury, such as a negligent contractor, defective equipment manufacturer, or another company’s employee. Ohio law allows injured workers to pursue third-party claims alongside workers’ comp without losing workers’ comp benefits, though the BWC may recover some costs from any third-party settlement you receive. An equipment malfunction, unsafe premises maintained by an outside vendor, or a vehicle accident involving another driver all create third-party liability exposure. These claims require proving negligence and causation through evidence like accident reports, witness statements, and expert analysis, making legal representation essential.
Vocational Rehabilitation and Return-to-Work Programs
Vocational rehabilitation programs through the BWC help you return to work through retraining, job placement assistance, and wage subsidies if your injury prevents your original job. The BWC’s transitional work bonus program offers incentives when employers create modified-duty positions, reducing your financial loss during recovery. These programs (when properly utilized) accelerate your path back to earning capacity while maintaining income support during the transition. The combination of third-party claims, SSDI applications, and vocational services creates multiple income streams that work together to maximize your total recovery rather than relying solely on workers’ comp benefits.
How to Maximize Your Claim and Handle Denials
File Your Claim with Precision and Speed
Filing a workers’ compensation claim in Ohio requires precision because the MCO and BWC scrutinize every submission for completeness and accuracy. Report your injury to your supervisor immediately-the same day if possible-because delays create documentation gaps that the MCO later uses against you. Your employer must file the First Report of Injury within 10 days of learning about your injury, but you should not wait for them to act. Contact the Ohio Bureau of Workers’ Compensation directly through their website or call to initiate your claim in parallel, which creates a paper trail showing you reported promptly.
Gather specific documentation before filing: the exact time and location of your injury, names and contact information for any witnesses, photos of the hazard or equipment involved, and your medical records from the initial treatment. The MCO bases its acceptance decision partly on whether your description matches medical findings, so consistency matters enormously. If you waited weeks to seek treatment, the MCO will argue your injury was not as severe as claimed or question whether it was work-related at all.

Build Strong Medical Evidence
Medical evidence from a BWC-certified provider strengthens your position because these providers understand workers’ comp requirements and document injuries in ways the MCO recognizes. Request copies of all documents the MCO submits to the BWC, including medical reports and claim decisions, because errors in these documents directly affect your benefits. The Industrial Commission of Ohio reports that claim denials often stem from incomplete initial filings or missing medical documentation, which means thorough preparation during filing prevents costly appeals later.
Appeal Denials With Targeted Evidence
Denials happen frequently-the BWC does not approve every claim automatically-but the appeals process reverses many denials when you submit proper evidence and challenge the denial basis specifically. The MCO or BWC must provide written reasons for denial, and you have 14 days to request a hearing before an Administrative Law Judge at the Industrial Commission of Ohio. Do not let this deadline pass because missing it forfeits your right to appeal.
Your appeal succeeds when you present medical evidence contradicting the denial reason, witness testimony supporting work-relatedness, or documentation showing the MCO misapplied the law. For example, if the BWC denied your claim claiming insufficient proof of work-relatedness, submit medical records linking your condition to your job duties, employer communications acknowledging the incident, or surveillance footage if available. Many workers lose appeals because they submit vague medical statements rather than detailed reports addressing the specific denial reasons.
Navigate the Hearing Process Effectively
An Administrative Law Judge will schedule a hearing within 60 to 90 days of your appeal request, which gives you time to gather evidence. Legal representation at the hearing stage dramatically improves outcomes because attorneys know which evidence persuades judges and how to cross-examine MCO representatives effectively. Workers representing themselves at hearings frequently fail to ask the right questions or present evidence in the order judges expect, which undermines their credibility.
The Industrial Commission publishes hearing decisions online, allowing you to review how judges have ruled on similar injuries in your region, which reveals what evidence actually persuades them. This research informs your strategy before the hearing and shows you which arguments succeed with judges in your area.
Final Thoughts
Ohio’s injury compensation alternatives extend far beyond traditional workers’ comp, and understanding each option determines whether you recover fully or accept inadequate benefits. You can pursue Temporary Total Disability for immediate wage replacement, Permanent Partial Disability for lasting impairment, Social Security Disability Insurance for long-term income security, and third-party liability claims when negligence caused your injury. Vocational rehabilitation programs accelerate your return to work while maintaining financial support during recovery, and these pathways work together rather than in isolation.
Speed and documentation separate successful claims from denied ones throughout the entire process. File your First Report of Injury within days of your workplace incident, gather witness information immediately, and obtain medical records from a BWC-certified provider so the MCO cannot question your timeline or medical findings. If the BWC denies your claim, appeal within 14 days and present medical evidence that directly addresses the denial reason, since many workers lose appeals by submitting weak documentation rather than targeted evidence.
Legal representation matters most when facing denials or navigating hearings before an Administrative Law Judge. We at Robin J Peterson Company, LLC represent injured workers throughout Ohio’s workers’ compensation system and fight to secure the benefits you deserve. Contact us today to discuss your claim and explore every injury compensation alternative available to you.
